Medical coding systems play a vital role in healthcare documentation, insurance billing, and public health reporting. Yet many healthcare professionals still ask the same question:
What’s the difference between ICD-10, ICD-10-CM, and ICD-11?
Although these terms are closely related, they represent different versions and adaptations of the International Classification of Diseases (ICD). Understanding these distinctions is essential for medical practices, especially in the United States, where accurate diagnosis coding directly impacts insurance claims, reimbursement, regulatory compliance, and healthcare analytics.
For physicians, practice managers, and revenue cycle teams, confusion around medical coding systems can lead to several operational and financial challenges, including:
- Claim denials
- Billing and coding errors
- Delayed reimbursements
- Compliance risks
In this guide, we explain the key differences between ICD-10, ICD-10-CM, and ICD-11 and what they mean for modern medical practices.
You will learn:
- What each coding system is and how it works
- Why the United States uses ICD-10-CM instead of ICD-10
- How ICD-11 differs from earlier coding systems
- Whether the United States is likely to adopt ICD-11 in the future
- How medical practices can prepare for future coding changes
By the end of this article, you will have a clear understanding of how these coding systems affect medical billing, clinical documentation, and healthcare data management, helping your practice improve coding accuracy and reduce claim denials.
What Are ICD Codes and Why Do They Matter in Healthcare?
ICD codes play a critical role in the daily operations of healthcare organizations. They ensure that patient diagnoses are documented accurately and that healthcare services can be billed correctly.
Without standardized diagnosis codes, healthcare systems would struggle to track diseases, process insurance claims, and analyze health data effectively.
Key Uses of ICD Codes in Healthcare
ICD codes support several essential healthcare functions.
Medical Documentation
Physicians use ICD codes to document patient diagnoses in electronic health records (EHRs). Accurate diagnosis coding helps ensure consistent patient records and supports effective clinical decision-making.
Insurance Billing and Reimbursement
Insurance providers rely on ICD diagnosis codes to determine whether medical services are medically necessary and eligible for reimbursement. Correct coding helps reduce claim denials and ensures timely payments.
Public Health Monitoring
Public health agencies use ICD-coded data to track disease outbreaks, monitor population health trends, and develop health policies.
Healthcare Analytics
Hospitals and medical practices analyze ICD data to identify trends in patient populations, treatment outcomes, and healthcare utilization. These insights help organizations improve care quality and operational efficiency.
Clinical Research
Researchers use ICD classifications to study disease prevalence, evaluate treatment effectiveness, and support medical innovation.
For additional details, visit the World Health Organization ICD classification portal:
https://www.who.int/standards/classifications/classification-of-diseases
What Is ICD-10?
ICD-10 is the 10th revision of the International Classification of Diseases, developed by the World Health Organization (WHO). This global system standardizes how diseases, injuries, and health conditions are classified and recorded across healthcare systems.
Introduced internationally in 1994, ICD-10 replaced the earlier ICD-9 classification system and significantly expanded the level of detail available for diagnosis coding.
Healthcare providers use ICD-10 codes to classify medical conditions using standardized diagnostic codes. These codes support essential healthcare functions such as clinical documentation, insurance billing, public health reporting, and medical research.
Key Features of ICD-10
Compared with previous versions, ICD-10 introduced a more detailed and structured approach to disease classification.
Key characteristics of ICD-10 include:
- Approximately 14,000 diagnostic codes
- Alphanumeric code structure that allows greater specificity
- Expanded disease classification categories
- Detailed codes for injuries and external causes of illness
- Organization into 22 disease chapters
These chapters cover major medical categories such as:
- Infectious diseases
- Cardiovascular conditions
- Respiratory disorders
- Endocrine diseases
- Mental health disorders
- Injuries and trauma
This expanded classification system allows healthcare professionals to document patient conditions with greater accuracy and clinical detail.
Limitations of ICD-10
Although ICD-10 represented a major improvement over earlier coding systems, it was originally developed during a time when healthcare relied heavily on paper-based documentation systems.
As healthcare technology evolved, several limitations became apparent.
Key challenges with ICD-10 include:
- Limited compatibility with modern digital health systems
- Difficulty capturing complex or multi-factor medical conditions
- Reduced flexibility for advanced healthcare data analytics
These limitations contributed to the development of ICD-11, the newest revision of the International Classification of Diseases, which was designed specifically for modern digital healthcare environments.
What Is ICD-10-CM?
In the United States, healthcare providers do not use the global ICD-10 classification system directly. Instead, they use an expanded version known as ICD-10-CM.
ICD-10-CM stands for:
International Classification of Diseases, 10th Revision, Clinical Modification
This system was developed specifically for the U.S. healthcare system and is maintained by the National Center for Health Statistics (NCHS) under the Centers for Disease Control and Prevention (CDC).
Healthcare providers use ICD-10-CM codes to document patient diagnoses and support critical processes such as medical billing, insurance claims, clinical documentation, and healthcare data reporting.
Official ICD-10-CM resources are available through the CDC:
https://www.cdc.gov/nchs/icd/icd-10-cm/index.html
Why ICD-10-CM Was Created
The original ICD-10 classification did not provide enough clinical detail to meet the complex billing and reporting requirements of the U.S. healthcare system.
To address this gap, ICD-10-CM was developed to:
- Expand diagnostic specificity
- Support medical billing and insurance reimbursement processes
- Improve clinical documentation accuracy
- Enhance healthcare data collection and reporting
These improvements help healthcare providers capture more detailed diagnostic information, which supports better clinical decision-making and more accurate claims processing.
Key Features of ICD-10-CM
ICD-10-CM significantly expands the number and specificity of diagnosis codes available to healthcare providers.
Key characteristics include:
- More than 70,000 diagnosis codes
- Greater clinical detail compared with ICD-10
- Laterality indicators to identify left or right side of the body
- Expanded injury and condition classifications
- Encounter type indicators that specify initial, subsequent, or sequela visits
Example ICD-10-CM code:
E11.9 — Type 2 diabetes mellitus without complications
This expanded code structure allows healthcare providers to document diagnoses with greater precision, helping insurers evaluate claims more accurately and reducing the risk of billing errors.
When the United States Adopted ICD-10-CM
The United States officially implemented ICD-10-CM on October 1, 2015, replacing the previous ICD-9-CM coding system.
Today, all HIPAA-covered healthcare providers must use ICD-10-CM for diagnosis coding when submitting insurance claims.
Accurate use of ICD-10-CM codes plays a critical role in medical billing, compliance, and revenue cycle management for healthcare organizations.
What Is ICD-11?
ICD-11 is the latest revision of the International Classification of Diseases, developed by the World Health Organization (WHO). It represents the newest global standard for classifying diseases, injuries, and health conditions.
The World Health Assembly approved ICD-11 in 2019, and it officially came into effect worldwide in 2022. Compared with earlier versions, ICD-11 was designed specifically for modern digital healthcare environments, making it easier to integrate with electronic systems and health data platforms.
Healthcare organizations can explore the full ICD-11 classification using the WHO ICD browser:
https://icd.who.int
Key Features of ICD-11
ICD-11 introduces several major improvements over previous versions of the classification system. These updates improve how healthcare providers document diagnoses, analyze health data, and share medical information across digital systems.
Digital-First Architecture
Unlike earlier versions, ICD-11 was designed with digital healthcare systems in mind. It integrates more easily with modern technologies such as:
- Electronic health records (EHRs)
- Healthcare analytics platforms
- Health information exchanges (HIEs)
- Digital health applications and tools
This digital-first design improves interoperability and allows healthcare organizations to manage medical data more efficiently.
Cluster Coding
ICD-11 introduces cluster coding, which allows healthcare providers to combine multiple codes to describe complex medical conditions more accurately.
This approach provides greater clinical detail and supports more precise documentation of patient diagnoses.
Expanded Disease Coverage
ICD-11 expands disease classification to better reflect modern healthcare challenges. The system includes improved coding for:
- Rare diseases
- Antimicrobial resistance
- Emerging infectious diseases
- Mental health and behavioral conditions
These updates help healthcare systems track evolving health trends and improve disease surveillance worldwide.
Improved Healthcare Data Analysis
ICD-11 supports advanced healthcare analytics and improved population health reporting. The enhanced structure allows researchers, healthcare providers, and policymakers to analyze health data more effectively.
Because of these improvements, ICD-11 is better suited for AI-driven healthcare systems, digital health technologies, and modern clinical data management.
ICD-10 vs ICD-10-CM vs ICD-11: Key Differences
Understanding the differences between ICD-10, ICD-10-CM, and ICD-11 is essential for healthcare providers, medical coders, and practice administrators. Each system serves a different role in disease classification and diagnosis coding.
The table below highlights the major differences between these three coding systems.
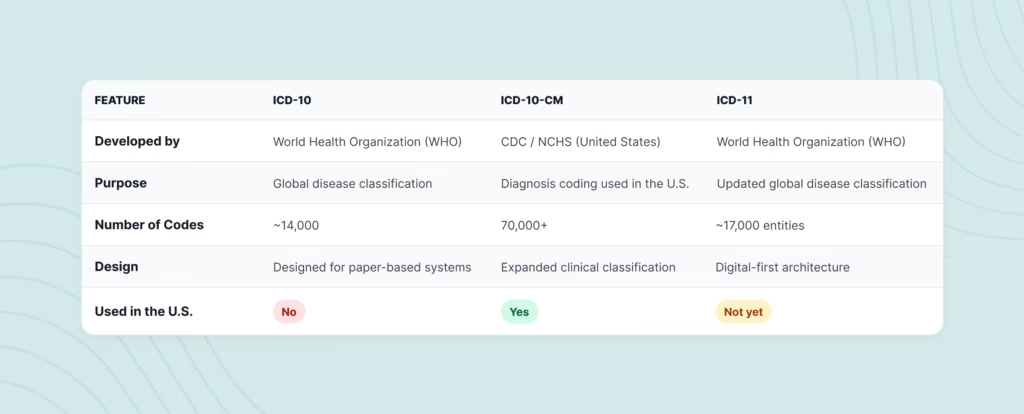
Key Takeaways
The comparison highlights several important points about these medical coding systems.
- ICD-10 serves as the global foundation for classifying diseases and health conditions.
- ICD-10-CM is the U.S. clinical modification used for diagnosis coding and insurance claims.
- ICD-11 represents the next generation of medical classification systems designed for modern digital healthcare environments.
Understanding these differences helps healthcare organizations improve diagnosis coding accuracy, medical billing processes, and healthcare data reporting.
Why the United States Uses ICD-10-CM Instead of ICD-10
The U.S. healthcare system requires more detailed diagnosis codes than the global ICD-10 classification system provides. To meet these needs, the United States adopted ICD-10-CM, an expanded version of ICD-10 designed specifically for American healthcare billing, compliance, and reporting requirements.
ICD-10-CM allows healthcare providers to document diagnoses with greater accuracy, which supports more reliable insurance claims processing and better healthcare data analysis.
Key Reasons for the U.S. Modification
Several factors led to the development of ICD-10-CM for the United States.
Expanded Diagnostic Detail
ICD-10-CM contains more than 70,000 diagnosis codes, compared with approximately 14,000 codes in ICD-10. This expanded code set allows healthcare providers to document medical conditions with greater precision.
More detailed diagnosis coding helps improve clinical documentation and claims accuracy.
Insurance Billing Requirements
The U.S. healthcare system relies heavily on detailed diagnosis coding for insurance billing and reimbursement.
Insurance companies use diagnosis codes to determine whether medical services are medically necessary and eligible for payment. ICD-10-CM provides the level of specificity required for these complex billing processes.
Clinical Specificity
ICD-10-CM supports more detailed clinical documentation by capturing additional information about a patient’s condition, including:
- Disease severity
- Complications
- Type of medical encounter
- Laterality (left or right side of the body)
This level of detail helps healthcare providers document patient conditions more accurately.
Healthcare Data Reporting
Healthcare organizations depend on detailed coding data to support a wide range of reporting and analysis activities.
ICD-10-CM enables more accurate data collection for:
- Quality reporting programs
- Population health monitoring
- Public health research
These capabilities help healthcare leaders, policymakers, and researchers better understand disease trends and healthcare outcomes.
Will the United States Adopt ICD-11?
Many healthcare professionals are asking an important question: When will the United States adopt ICD-11?
At present, ICD-10-CM remains the official diagnosis coding system used in the U.S. healthcare system. While ICD-11 has been implemented globally, U.S. health authorities have not announced an official timeline for transitioning from ICD-10-CM to ICD-11.
Because ICD-10-CM already provides a highly detailed diagnosis coding framework, healthcare organizations in the United States continue to rely on this system for medical billing, clinical documentation, and insurance claims processing.
Challenges of ICD-11 Adoption in the U.S.
Transitioning to ICD-11 would require significant changes across the U.S. healthcare infrastructure. Healthcare providers, insurers, and technology vendors would all need to update their systems and processes.
Key challenges include:
- Updating electronic health record (EHR) systems
- Modifying billing software and revenue cycle management platforms
- Adapting payer claims processing systems
- Training medical coders, physicians, and billing staff on the new coding structure
Because these updates would require extensive planning and investment, many experts believe that a full transition to ICD-11 in the United States may still be several years away.
In the meantime, healthcare organizations continue to focus on improving ICD-10-CM coding accuracy and compliance within their existing systems.
How ICD Coding Systems Impact Medical Practices
Accurate ICD diagnosis coding plays a critical role in the financial and operational success of medical practices. Proper use of ICD codes ensures that patient conditions are documented correctly and that healthcare providers receive appropriate reimbursement for the services they deliver.
When diagnosis coding errors occur, medical practices may experience several costly issues.
Common Problems Caused by Diagnosis Coding Errors
Incorrect or incomplete ICD codes can disrupt the medical billing process and lead to financial losses. Common problems include:
- Claim denials from insurance providers
- Delayed reimbursements for medical services
- Increased compliance and audit risks
- Revenue leakage due to inaccurate billing
Even when a treatment is medically necessary, insurers may reject a claim if the diagnosis code does not fully justify the service provided.
Benefits of Accurate ICD Coding
Improving diagnosis coding accuracy helps medical practices strengthen their revenue cycle and operational efficiency. Accurate ICD coding can help practices:
- Increase insurance claim approval rates
- Reduce billing errors and payment delays
- Maintain regulatory compliance
- Generate more reliable healthcare data insights
By focusing on accurate coding practices, healthcare organizations can improve both financial performance and clinical data quality.
How Medical Practices Can Prepare for Future Coding Changes
Although ICD-11 adoption in the United States may still be several years away, healthcare organizations can begin preparing now. Taking proactive steps helps medical practices stay compliant with evolving coding standards and adapt more easily to future changes in diagnosis coding systems.
Invest in Coding Education
Regular training helps medical coders, billing teams, and clinical staff stay current with evolving ICD coding guidelines and documentation requirements. Ongoing education improves coding accuracy and reduces the risk of billing errors.
Monitor Regulatory Updates
Healthcare providers should stay informed about regulatory updates and coding changes from key healthcare organizations, including:
- Centers for Disease Control and Prevention (CDC)
- Centers for Medicare & Medicaid Services (CMS)
- World Health Organization (WHO)
Tracking these updates helps practices prepare for potential changes to diagnosis coding standards.
Upgrade Technology Systems
Modern electronic health record (EHR) and practice management systems should support flexible coding frameworks and future classification updates. Updating healthcare technology infrastructure can make future transitions, such as a potential move to ICD-11, much easier to manage.
Use Healthcare Analytics Tools
Healthcare analytics platforms can help organizations monitor coding trends, billing performance, and revenue cycle efficiency. These tools identify coding inconsistencies, billing inefficiencies, and potential revenue losses, allowing practices to improve financial and operational outcomes.
Improve Coding Accuracy and Revenue Insights
Accurate diagnosis coding is essential for maximizing claim approvals, ensuring proper reimbursement, and maintaining the financial health of a medical practice. Even small coding errors can result in claim denials, delayed payments, compliance risks, and significant revenue loss.
At Medviz Systems, we provide end-to-end medical billing and coding support that helps practices:
- Improve coding accuracy and compliance
- Reduce claim denials and rejections
- Accelerate reimbursements and cash flow
- Optimize revenue cycle performance
- Gain clear insights into billing and operational performance
Our team works closely with medical practices to manage the entire revenue cycle, from coding and claim submission to denial management and reporting, allowing providers to focus on delivering quality patient care.
Start your free consultation today:
Phone: +1 (727) 214-2749
Email: success@medviz.ai

