Primary care practices across the United States are already under pressure from staffing shortages, rising administrative burdens, and tighter reimbursement margins. Now, a new challenge is drawing attention across the healthcare industry: AI-powered insurance denials.
While insurers have long used technology in claims review and utilization management, physicians and policy experts are increasingly concerned that AI and automated decision tools are making prior authorization and coverage denials faster, less transparent, and harder to fight. For primary care providers, that can mean delayed treatment, more staff time spent on payer follow-up, and more pressure on already strained revenue cycle operations [1].
This matters because primary care sits at the center of the patient journey. From referrals and diagnostic testing to chronic care management and medication approvals, primary care practices often absorb the first wave of payer friction. When denials increase, the impact is felt not only in patient care but also in cash flow, staff productivity, and patient satisfaction.
In this article, we explain what AI-powered insurance denials are, why they matter for primary care practices, how they affect revenue cycle management, and what providers can do now to reduce risk and strengthen reimbursement performance.
What Are AI-Powered Insurance Denials?
The term AI-powered insurance denials generally refers to the use of artificial intelligence, predictive analytics, or automated decision-support tools by insurers during prior authorization, utilization review, or coverage determination workflows. Recent reporting and policy analysis show these tools are increasingly being discussed in connection with medical necessity review, prior authorization, and adverse determinations [1], [5].
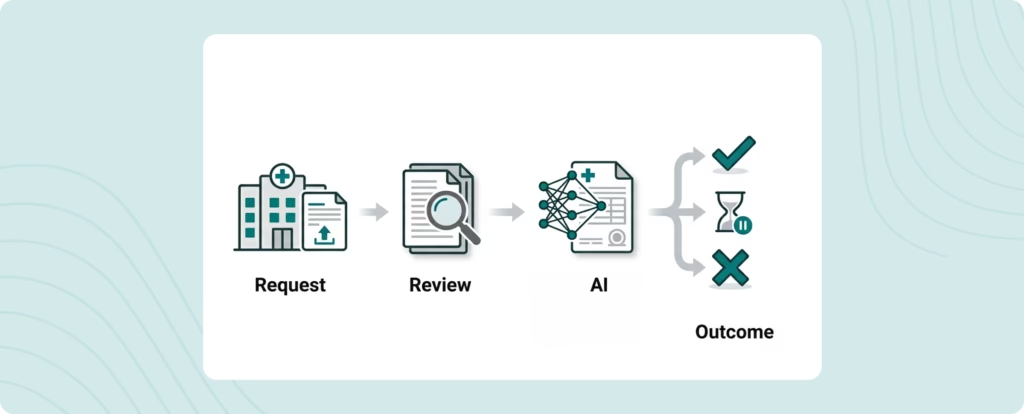
In plain language, these tools may be used to:
- Flag requests for further review
- Sort or prioritize cases
- Recommend approval or denial outcomes
- Identify high-cost services for closer scrutiny
- Accelerate adverse determinations
It is important to separate a few related concepts:
- Claim denials: rejection of submitted claims for payment
- Prior authorization denials: refusal to approve services before they are performed
- Medical necessity reviews: evaluation of whether a treatment or service meets payer criteria
- Algorithm-assisted utilization management: use of automated tools to guide insurer review decisions
Most of the recent concern in healthcare reporting has focused on prior authorization and medical necessity review, rather than simple back-end claims edits. That distinction matters because prior authorization denials can stop care before it happens, creating immediate disruption for both patients and practices [1].
For primary care groups, this means payer automation is no longer just a billing department issue. It is becoming a broader access, workflow, and reimbursement issue.
Why Primary Care Practices Are Especially Vulnerable
Primary care practices are especially exposed to denial risk because they manage a wide range of services across a broad payer mix. A PCP may coordinate preventive care, specialist referrals, imaging, lab work, medications, and chronic disease treatment all in the same week, often under different payer rules.
That creates several layers of vulnerability:
- High patient volumes
- Frequent referral and authorization requirements
- Diverse plan policies across Medicare, Medicare Advantage, Medicaid managed care, and commercial payers
- Smaller administrative teams compared with large health systems
- Less internal bandwidth for appeals and payer follow-up
Unlike some specialty practices that focus on narrower service lines, primary care must navigate multiple denial triggers at once. A delay in referral approval, a rejected imaging request, or a medication prior authorization hold can all create downstream clinical and financial consequences.
This is one reason primary care revenue cycle management has become more complex. Denials no longer affect only reimbursement after the visit. They can interfere with patient scheduling, care coordination, treatment adherence, and provider efficiency before a claim is even submitted.
The Evidence Behind Growing Concerns About AI in Prior Authorization
Concern about AI prior authorization denials is not just anecdotal. Physician survey data and policy reporting suggest that worry is rising across the industry.
According to the American Medical Association, 61% of physicians said they were concerned that health plans’ use of AI was increasing prior authorization denials [2].
That concern is highly relevant to primary care because an AJMC summary of the 2024 AMA survey reported that the sample included 1,000 practicing U.S. physicians, with 40% primary care physicians and 60% specialists [3].
Additional survey findings show why the issue matters so much operationally:
- 93% of physicians said prior authorization delays patient care
- 82% said it can lead to treatment abandonment
- 94% said it has a somewhat or significantly negative impact on patient clinical outcomes
- 29% said prior authorization caused a serious adverse event for a patient in their care
- Physicians reported completing an average of 39 prior authorizations per week and spending about 13 hours weekly on the process [3]
For primary care practices, these figures translate into more administrative work, more delayed care, and more strain on front-desk, clinical, and billing teams.
The bigger issue is not just that AI exists in payer workflows. It is that many physicians and researchers worry these tools may be used with limited transparency and insufficient human oversight. Stanford’s summary of a Health Affairs article noted concerns that wrongful denials may be occurring because of a lack of meaningful human review of AI recommendations [4].
How AI-Powered Denials Impact Patient Care and Practice Revenue
The consequences of insurance denials in primary care go far beyond a single unpaid claim. When denial activity rises, the damage shows up in four major areas.
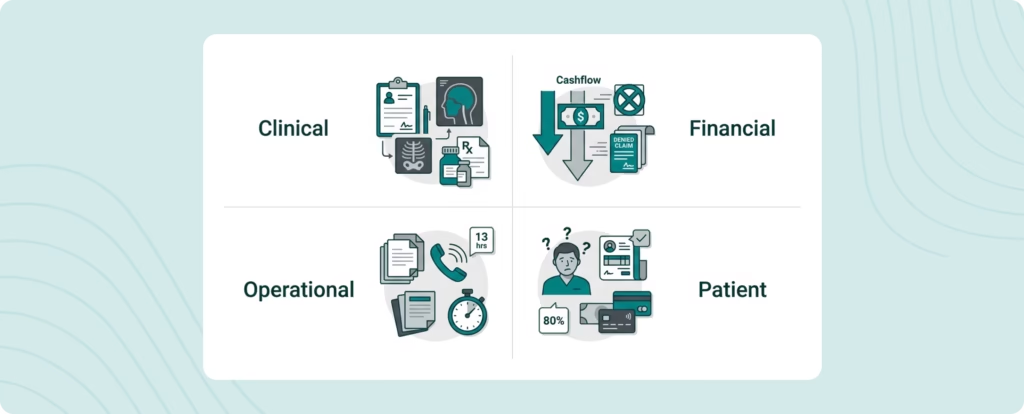
1. Clinical Consequences
A delayed or denied authorization may postpone:
- Diagnostic imaging
- Specialist referrals
- Medications
- Procedures
- Ongoing treatment plans
For patients with chronic conditions, even a short delay can disrupt continuity of care. For preventive services, delay may reduce follow-through entirely. Survey data cited by AJMC found that delays caused by prior authorization are associated with treatment abandonment, negative clinical outcomes, and serious adverse events [3].
2. Financial Consequences
Denied or delayed approvals often lead to:
- Slower reimbursement
- Increased accounts receivable days
- More write-offs
- More unpaid staff labor
- Higher cost per collected dollar
This is where denial management for primary care becomes critical. Every denial represents rework, and rework erodes margin.
3. Operational Consequences
Staff must spend more time on:
- Resubmissions
- Payer calls
- Documentation gathering
- Medical necessity support
- Appeals
AJMC’s summary of the AMA survey reported that physicians spend about 13 hours per week on prior authorization-related work, highlighting the scale of the administrative burden [3].
4. Patient Experience Consequences
Patients may experience:
- Confusion about coverage
- Frustration over delays
- Unexpected out-of-pocket exposure
- Loss of trust in the practice
- Abandonment of recommended care
AJMC also reported that 80% of physicians said prior authorization delays or denials sometimes force patients to pay out of pocket for medication [3].
What Recent Lawsuits and Policy Developments Mean for Providers
Legal and regulatory attention is growing around insurer use of AI in healthcare decision-making.
Healthcare Finance News reported on a class action lawsuit involving UnitedHealth and subsidiary naviHealth in which plaintiffs alleged that the AI program nH Predict was used in post-acute care benefit denials, at times superseding physician judgment. The report says plaintiffs alleged a 90% error rate, meaning nine out of ten appealed denials were ultimately reversed. These are allegations from litigation, not final court findings on the merits [6].
At the federal level, KFF Health News reported that CMS planned a Medicare pilot called WISeR that would test the use of an AI algorithm in prior authorization decisions for some Medicare services in Arizona, Ohio, Oklahoma, New Jersey, Texas, and Washington, beginning January 1, 2026, and running through 2031. KFF also reported that CMS said no Medicare request would be denied before review by a qualified human clinician and that vendors would be barred from compensation arrangements tied to denial rates [1].
At the state level, the Kansas Legislative Research Department’s 2026 briefing book noted that Texas SB 815 prohibits the use of AI to make adverse determinations regarding the medical necessity of services, limiting AI use to administrative support or fraud detection and permitting regulatory inspection of payer AI tools [5].
Together, these developments show that AI in payer decision-making is attracting scrutiny from physicians, regulators, and lawmakers.
Warning Signs Your Practice May Already Be Feeling the Effects
Many practices may already be seeing the signs without labeling them as AI-related. If your team has noticed any of the following, payer automation may be part of the story:
- Rising denial rates for medically necessary services
- More repeated requests for medical records or documentation
- Slower approval turnaround times
- Inconsistent payer decisions for similar cases
- Higher staff time spent on follow-up and appeals
- More patient complaints about delays
- Increased write-offs tied to unresolved denials
These warning signs should not be ignored. They are often indicators that payer rules, review criteria, or workflow automation have become more aggressive.
What Primary Care Practices Need to Do Now
The most effective response to AI-powered insurance denials is operational discipline. Practices need stronger front-end controls, better documentation, tighter workflows, and more structured denial follow-up.

Strengthen Front-End Insurance Verification
Before the visit, practices should:
- Verify eligibility and active coverage
- Confirm benefits and plan limitations
- Validate referral requirements
- Check authorization rules for payer-specific services
- Identify high-risk services likely to trigger review
Improve Documentation for Medical Necessity
Clinical documentation should clearly support:
- Diagnosis and symptoms
- Severity and duration
- Prior treatment attempts
- Rationale for ordered service
- Need for referral, medication, or testing
Standardize Prior Authorization Workflows
Primary care practices should avoid ad hoc authorization handling. Instead, use structured workflows with:
- Payer-specific checklists
- Service-based routing
- Turnaround-time tracking
- Escalation timelines
- Centralized status visibility
Build a Stronger Denial Management Process
A proactive appeals strategy should include:
- Categorizing denials by root cause
- Prioritizing high-value denials
- Attaching complete supporting documentation
- Tracking appeal outcomes by payer
- Identifying repeat denial patterns
Monitor Denial Analytics Closely
Every primary care practice should track key performance indicators such as:
- Denial rate by payer
- First-pass resolution rate
- Authorization turnaround time
- Appeal success rate
- Days in accounts receivable
- Write-off volume by denial category
These steps become even more important in light of survey findings showing the scale of care delays, treatment abandonment, negative clinical outcomes, and physician burden tied to prior authorization [2], [3].
Why Outsourced Medical Billing and RCM Can Help
For many practices, especially independent groups and growing clinics, the reality is simple: internal teams are already overloaded. That is why outsourced medical billing for primary care has become a strategic option rather than just an administrative convenience.
A strong RCM partner can help practices:
- Reduce claim and authorization errors
- Manage payer-specific requirements
- Improve coding and documentation alignment
- Track denials and appeals more consistently
- Provide visibility into denial trends and reimbursement performance
- Reduce administrative burden on in-house staff
Given the AMA and AJMC findings on high physician burden and care disruption from prior authorization, stronger RCM support can help practices respond more consistently and protect revenue [2], [3].

Conclusion
AI-powered insurance denials are becoming a growing concern for U.S. primary care practices because they may make prior authorization and coverage review faster, less transparent, and more difficult to challenge. Physicians are increasingly worried about AI-driven denials, and policymakers are beginning to respond [2], [5].
The good news is that practices are not powerless. Stronger eligibility checks, better documentation, standardized prior authorization workflows, disciplined denial management, and smarter RCM support can all reduce the impact.
Start Reducing Denials Today
AI-powered denials and prior authorization delays can quickly impact your cash flow and staff productivity. Medviz Systems helps primary care practices improve billing accuracy, reduce denials, and strengthen revenue cycle performance.
Get Free Revenue Leakage Audit Today
Phone: +1 (727) 214-2749
Email: success@medviz.ai
References
[1] https://kffhealthnews.org/news/article/ai-medicare-prior-authorization-trump-pilot-program-wiser/
[4] https://news.stanford.edu/stories/2026/01/ai-algorithms-health-insurance-care-risks-research
[5] https://klrd.gov/2026/03/02/briefing-book-2026-artificial-intelligence-use-in-health-insurance/


Leave a Reply